So I had paeds 1 yesterday. The day before, at around 9:00, everyone who were to have the exam got an email stating the examiner and the time of everyone’s exam. Our examiner was to be Dr. András Tárnok, and my time was 9:10. According to the email, we were to call the examiner at our designated time. There were 20 minutes between each student’s time, so we knew upfront that each exam would last maximum 20 minutes.
So 9:10 yesterday, I called him on Teams, and he answered. He asks my ID, which of my names to use and whether I’m in Hungary.
He holds up the cards with the neonatology topics in a fan-shape. He asks me where to pick from. I tell him to pick somewhere in the middle, and out comes the first topic: “Persistant pulmonary hypertension of the newborn. Patent ductus arteriosus.” He asks me if it’s alright, to which I reply that it is.
- Examiner: Can you start with the second part? Patent ductus arteriosus?
- Me: Okay, so the ductus arteriosus is an embryonic structure which connects the truncus arteriosus with the aortic arch, so it allows blood to avoid the lungs in embryonic life. Persistant ductus arteriosus is when it doesn’t close early after birth.
- *During these sentences he was writing something down, so he didn’t notice, or at least react to, my mistake regarding truncus arteriosus.*
- E: So is it good or bad?
- M: It’s not good, because, if it’s very small it might be asymptomatic, but if it’s large it may cause symptoms.
- E: What symptoms?
- M: For example, uhm, dyspnoea, or tachycardia.
- E: Okay.. Please tell me, where is this little blood vessel? What does it connect to?
- M: It connects the truncus arteriosus to the aortic arch.
- E: Truncus arteriosus?
- M: No, no, the pulmonary trunk, sorry.
- E: So there’s a connection between the pulmonary artery and the aorta. Now think about it, if you have a connection between the systemic and the pulmonary circulation by this little thing, what is going to happen?
- M: The pressure is higher in the aorta, so it’s like a left-to-right shunt.
- E: Okay, so what’s going to happen with the lungs then?
- M: They will experience more blood than they normally do
- E: So then what is going to happen?
- M: Pulmonary hypertension.
- E: Good. Do I need to ask questions or would you like to make sentences yourself?
- M: Well, I can try to make sentences but I appreciate some help if I need it.
- E: You’ve already received help. *we laugh*
- M: Yeah, so this is not a good thing, pulmonary hypertension is not a good thing. Uhm, where should I continue. It can be closed either pharmacologically or by percutaneous procedure. Pharmacologically you would use an NSAID like indomethacin or ibuprofen.
- E: Okay. Why do we indomethacin?
- M: It works because prostaglandins are what keep the ductus arteriosus open
- E: It’s much nicer to have it explained like that, so if you now it, just say it so. It’s so easy. Prostaglandins are what keep it open, so if I give something which inhibits prostaglandin synthesis, it will close. If that doesn’t help, we have the surgical option. If not percutaneous we must perform a thoracotomy and put a clip on there. Good. Clinically, what do you see apart from tachypnoea, or whatever. Is there anything else on physical exam?
- M: Uhm, they may experience respiratory distress.
- E: Is it the cause or the consequence?
- M: The consequence.. Uhm, on physical exam there is a murmur.
- E: Okay, we’re approaching. Tell me the characteristics of that murmur.
- M: I can’t recall actually..
- E: When do you hear it?
- M: After systole, I would suppose…
- E: Where does this murmur generate?
- M: Where? Oh, uhm, I would guess the turbulence in the pulmonary trunk?
- E: Ehm, we’re going down to basics, to year three now. So if we do auscultation at the heart, you know that different sounds are produced in different cycles of the heart-beat. In this scenario, what do you think?
- M: Second heard sound?
- E: What is the problem [of the PDA]? Nikolas, tell me. Where is the problem?
- M: The problem is the pulmonary hypertension.
- E: No, the problem is the connection between the two circulations by this tiny little blood vessel. This is the problem, this is the PDA, yeah? And where is this?
- M: Between the aortic arch and the pulmonary trunk.
- E: Is it outside or inside the heart?
- M: Outside.
- E: Okay. Does it have any connection to the valves?
- M: Uhm, no, not directly.
- E: Okay. So if it’s outside the heart, and it’s not connected to the valves, then what is the characteristics of this murmur? Because, in the heart, if we have a systolic murmur, or a diastolic murmur, it is connected to the phase where the heart is beating. And because the valves are open and then closing, this is going to give you the first and the second heart sounds, yeah?
- M: Yeah
- E: Now, this tiny blood vessel has no valves in it at all. So, how would you characterise it?
- M: Uhm..
- E: Does it have any relation to the heart cycle?
- M: Oh, uhm.. no, I would suppose not.
- E: No. So, what is the charactisterics of this murmur?
- M: So it’s constant throughout the heart cycle.
- E: It’s continuous. Because it is going to happen all the time, from the high-pressure area to the low-pressure area, and you will hear this sound because it’s a thin connection, therefore, when the blood is flowing through a narrow part, it is going to produce the sound. Where do you hear this? Is there a typical site where you can hear this?
- *Somehow it just occured to me*
- M: In the left infraclavicular region.
- E: Exactly, exactly. So if you suspect it you put your stethoscope there, and you try to hear. It’s called a continuous type of murmur. It doesn’t have an end, because there’s no valve to put an end to it, where the blood flow is stopped. Okay?
- M: Yeah.
- E: Okay, so now that I’ve explained you this topic, we need to move on to the second one, I don’t want you to get in trouble with the persistent pulmonary hypertension, okay? I do not wish to explain more of that. So all-together this is a 3 at the moment.
Not a great performance by me thus far, but he’d been very nice about it. We were around 11 minutes into the exam. He hold up the topics for general paediatrics and asks me where to draw from. I ask him for a card from the middle again, and he draws out the second topic, “diabetes mellitus”. “Is it better?”, he asks. “That is better”, I reply.
- E: Now. No interruptions, nice sentences, brief summary.
- M: Okay, so. In childhood, still diabetes type 1 is the most common, but of course type 2 is becoming more and more common, but I’ll focus on type 1. So type 1 is mostly an autoimmune phenomenon, where there’s autoimmune destruction of the beta cells causing them to have insulin deficiency. There are many antibodies involved in this, like anti-insular cell, anti-… Oh, well I guess I just remember that one. Glutamic acid something, there’s an enzyme, GAD or something. Okay, anyway. So a child may present with typical symptoms of diabetes type 1, or they can present with ketoacidosis. The typical symptoms of diabetes type 1 are weight loss, polydipsia, polyuria.
- *He hold up three fingers*
- E: Another “p”. [Like, another symptom on “p”]
- M: Uhm..
- E: They eat a lot.
- M: Sorry? [I couldn’t hear what he said]
- E: They eat a lot.
- M: Polyphagia.
- E: Exactly.
- M: Yeah, they have to make up for the lost glucose. And weight loss, even though they eat a lot. Or maybe they wouldn’t gain as much weight as their eating habits should’ve made them.
- *He nods*
- M: Okay, where was I? Symptoms, uhm.. So, the diagnosis can be made in multiple ways. Fasting plasma glucose, HbA1c, OGTT, random plasma glucose.
- E: Okay.
- M: So if the HbA1c is above 6,5%, or the fasting is above 7 mM, or the random is above 11,1 mM, or the OGTT is above 11,1 mM, all of those are diagnostic for diabetes.
- E: How do you determine that there’s no insulin?
- M: You look at the C-peptide level.
- E: What is that?
- M: Sorry?
- E: What is the C-peptide?
- M: The C-peptide is the peptide which is released simulatenously as insulin from the beta-cells.
- E: How? *slightly dissatisfied face*
- M: No, it’s actually a part of the prepeptide of insulin, which is cleaved off to make the C-peptide and the insulin.
- E: Exactly. Good. *very satisfied face* Treatment?
- M: The treatment is insulin injections.
- E: How? Once a life I give an injection and it’s done?
- M: Sorry?
- E: Is it like a jab? I give it once a life and it’s done?
- M: No, it’s daily. There are multiple regimens to do this. They often use once or twice a day a long-lasting insulin, and before meals that can take some short-acting insulin.
- E: Where do you give it?
- M: You give it in the abdominal fat.
- E: So how is it administered?
- M: With, uh…
- E: Or *where*?
- M: Oh, subcutaneous.
- E: Yes, okay. Why don’t we give IV?
- M: Well it’s because it’s much easier for the patient to inject themselves subcutaneous than IV.
- E: And, also? What is going to happen if you inject IV?
- M: Everything is immediately into the blood stream, so it won’t be released gradually from the subcutaneous fat.
- E: Okay. What is the prognosis of this medical condition? Are they going to be cured, ever?
- M: No, they’ll never be cured. They have to do this life-long. And the exact prognosis depends on how strict they are with maintaining normoglycaemia to the best of their ability. Most of them will develop some diabetic complications, microvascular or macrovascular. Diabetic retinopathy, neuropathy, nephropathy.
- E: Have you ever seen a type 1 diabetic patient?
- M: I have some friends who are, but I’ve never seen it in a patient, no.
- E: And your friends, just a personal question. Are they all right?
- M: Yes, they are.
- E: So they’re functioning well?
- M: Yeah.
- E: And that is the aim of the treatment. To have a normal life, kind of. What about restrictions in this medical problem?
- M: So they should try to eat almost a constant amount of carbohydrates, because the amount of carbohydrates they eat must be balanced out with the insulin they take.
- E: Okay. Have you heard of insulin that is somehow acting differently than the normal? That has an advantage nowadays in diabetic patients.
- M: Are you talking about like a pump?
- E: Pump is okay, yes, but anything else you have heard? Because you said, it has to be given the short-acting before the meal, yeah? What if I don’t feel like eating? I’m not hungry. And the insulin is already in my body. What’s going to happen?
- M: You would get hypoglycaemia.
- E: Can you give me any ideas what it can cause?
- M: In the worst case it could cause a coma, but in …
- E: And death.
- M: And death, yeah.
- E: So you lose consciousness, you’re going to have seizures. And you lose contact with the environment. Now, have you heard about so-called insulin analogues?
- M: Yeah.
- E: Insulin analogues are good because you can give them after the meal, because they’re much faster. So it can be paired with the carbohydrate input. So if you don’t know, because you have a bit of tummy pain or sickness-feeling, and you don’t feel like eating that much, you can balance it to the amount you have eaten. And it’s not going to disturb your blood sugar level that much. Okay. All right. Nikolas. That was 5. I’m happy. So all together, it’s a 4. Okay?
- M: Okay, yeah, I think that’s deserved.
- [I meant to say that that’s more than I deserved but I was so nervous and said the wrong thing]
- E: Okay, Nikolas, please look at those neonatal stuff, because we can lose patients with persistent pulmonary hypertension, or not discovered PDA can cause long-term problems. It’s a significant question which you’re going to fail at the final if you have big gaps, okay?
I said thank you, we wished each other a good day, and with that I was done with this exam period.
He was very nice and compassionate, and was smiling and nodding along during the whole exam. I’m glad I had him as my examiner, although I’ve heard that all examiners in paeds are very nice.
I had an amazing idea before this exam. I’d start an exercise session on my smartwatch so I could monitor my heart rate during the exam. I had to choose the type of exercise. I chose “gardening”, because “having exam” was not an option for some reason. Here are the results!
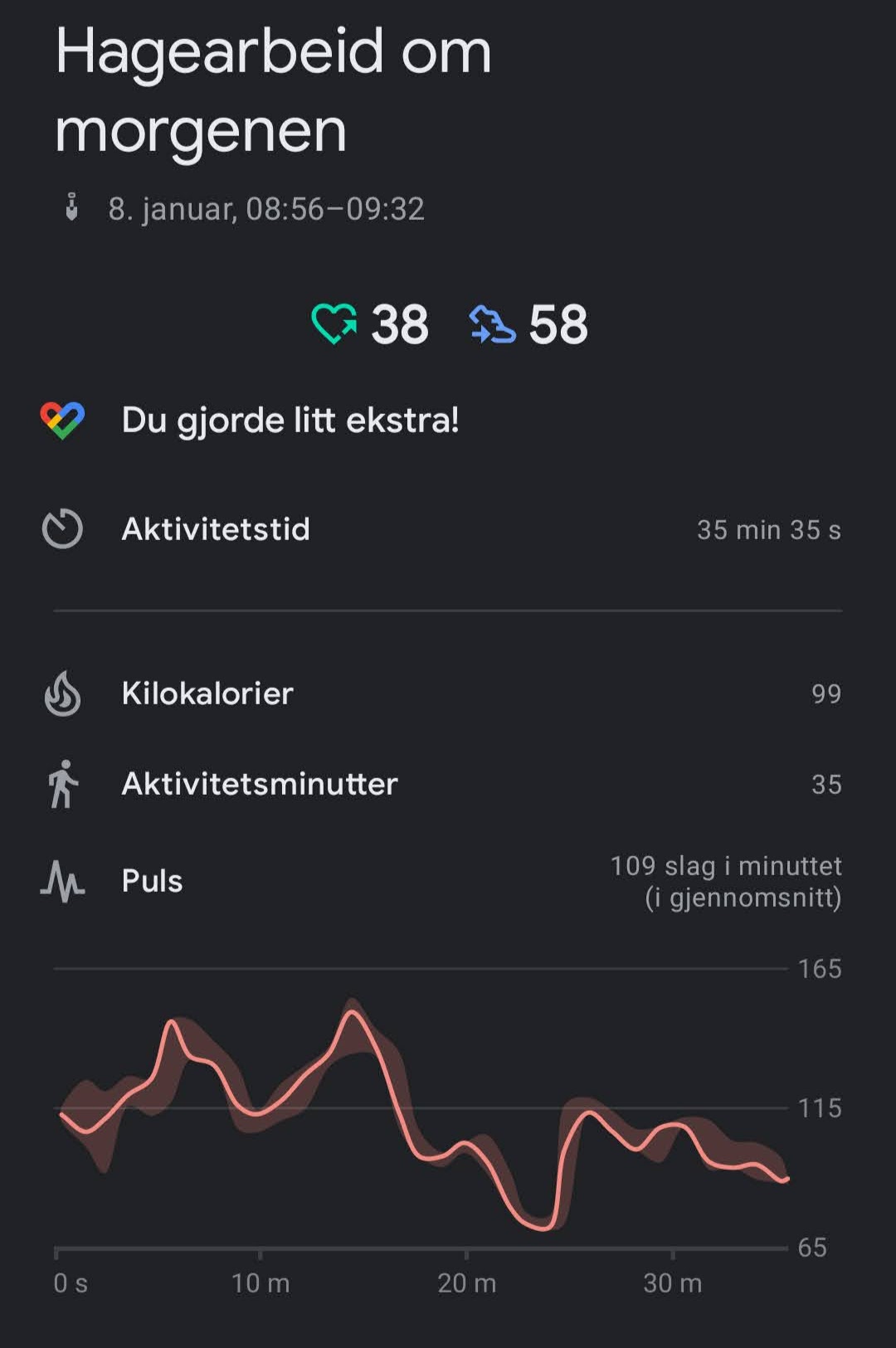
My “gardening session” started 08:56, 14 minutes before my exam started, so the exam started 14 minutes into the gardning. At that point, my heart rate peaked at a comfortable 155 bpm. I suppose the sudden drop was because of how calming the examiner was. I don’t know what happened toward 24 minutes; the HR sensor probably dysfunctioned. At around 25 minutes I drew my second topic. At around 33 minutes my exam was done. Fun stuff!
Now that I’m done with my exams I’ll upload my neuro and paeds 1 notes to the website as usual. At the end of exam period I’ll return with the fan-favourite: statistics (I promise!).
Good luck to those who aren’t finished yet, and congratulations to those who are finished!
Congrats 😄
Don’t you take Forensics orally to get a 5 😉 ?
Thank you! and haha, no way
Congratulations!!!
I’m really looking forward to the splendid statistics!
❤️