Table of Contents
Page created on October 18, 2018. Last updated on June 14, 2022 at 12:05
In the previous topic we saw some indirectly acting sympathomimetics. Now we’re going to look at some directly acting ones.
Overview of drugs
| Catecholamines | Selective α-receptor agonists | Selective β-receptor agonists | ||
| α1 selective | α2 selective | Non-subtype selective | β2 selective | |
| Dobutamine | Oxymetazoline | Clonidine | Ephedrine | Formoterol |
| Dopamine | Phenylephrine | Methyldopa | Salbutamol/albuterol | |
| Epinephrine | Xylometazoline | Dexmedetomidine | Salmeterol | |
| Isoprenaline | Tizanidine | Terbutaline | ||
| Norepinephrine | Vilanterol | |||
Adrenergic receptors
Adrenergic receptors, or adrenoceptors are the receptors that catecholamines can bind to. Seven types are important: α1, α2, β1, β2, β3, D1 and D2.
They’re all G-protein coupled receptors. Recall that depending on the type of G-protein on the inside of the cell will the activity of the receptor be different. Gs-type G-protein activates adenylyl cyclase, Gi type inhibits it and Gq type activates phospholipase C.
α1 receptor has a Gq type G-protein, meaning that when an agonist binds to it will phospholipase C be activated. The result will be activation of protein kinase C.
α2 receptor has Gi type G-protein, meaning it reduces the activity of adenylyl cyclase and therefore reduces the level of cAMP in the cell and inhibits protein kinase A. Recall from the previous topic that α2 receptor is part of the negative feedback, so it makes sense that it is inhibitory.
All β receptors are Gs coupled, meaning that they activate adenylyl cyclase and therefore increase the level of cAMP and activates protein kinase A.
Hint: An easy way to remember the G-proteins of α and β receptors is to remember the mnemonic “qiss”, which sounds almost like “kiss”. α1 has Gq, α2 has Gi, β1 has Gs and β2 has Gs.
D1 and D2 are the receptors for dopamine. D1 is Gs coupled as well and therefore activates protein kinase A. D2 is Gi coupled and therefore inactivates protein kinase A. D1 activates vasodilation of renal, splanchnic, coronary and cerebral vessels.
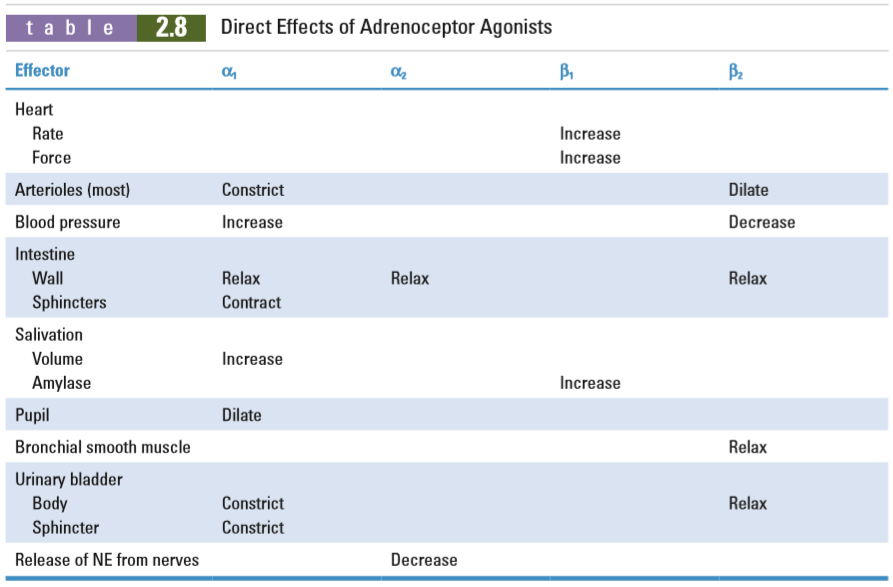
The most important takeaway from this table is that α1 receptors mainly cause vasoconstriction, β1 receptors mainly cause positive heart effects (chronotropy, inotropy) which increases cardiac output, and that β2 receptors mainly cause vasodilation and bronchodilation. Activation of α2 receptors decreases sympathetic outflow by decreasing noradrenaline (NE) transmission, thereby causing negative heart effects and vasodilation.
Not written in the table is the fact that β1 receptors stimulate renin release.
Catecholamines in clinical practice
Compounds
- Noradrenaline (norepinephrine)
- Adrenaline (epinephrine)
- Dopamine
- Dobutamine
- Isoprenaline
Vasopressors are drugs which induce peripheral vasoconstriction, thereby increasing systemic vascular resistance (SVR), which in turn increases blood pressure. Inotropes are drugs which increase cardiac contractility. Drugs of both types are important in haemodynamic instability, where there can be severe hypotension and the cardiac output may be insufficient.
Noradrenaline, adrenaline, dopamine, and isoprenaline (as well as vasopressin and phenylephrine) are vasopressors, but also inotropes to some degree. Dobutamine is a pure inotrope.
Indications and mechanism of action
Noradrenaline, adrenaline, dopamine, dobutamine, and isoprenaline are all used in the treatment of haemodynamic instability or shock. The exact drug to use depends on the type of shock and the desired effect, and is mostly the work of a specialised in intensive care.
Noradrenaline acts on mainly α1 and β1 receptors, producing vasoconstriction and positive heart effects.
Adrenaline has strong β1 activity and moderate β2 and α1 activity. In low doses the β1 activity predominates, causing inotropic and chronotropic effects but no vasoconstriction (as the β2-mediated vasodilation outweighs the α1-mediated vasoconstriction. In higher doses however, the alpha-adrenergic receptor effect predominates, causing vasoconstriction in addition to an increased CO.
Adrenaline is also the main treatment in anaphylactic shock. It can also be added to local anaesthetic solutions to increase their effect and topically to stop bleeding.
Dopamine acts on D1 and D2 receptors, as well as β and α receptors. The effect depends on the dose. Its use has mostly fallen out of favour as other cathecolamines are preferred instead.
Dobutamine has strong β1 effect and small α and β2 effects. This makes it increase the CO while causing peripheral vasodilation. This makes it especially useful in acute heart failure and cardiogenic shock.
Isoprenaline has β1 effect and β2 effect, giving it a predominantly chronotropic effect. This makes it useful in haemodynamic instability due to bradycardia.
Dosing
The dose of adrenaline in anaphylactic shock is 0.25 – 1 mg, while when used as a supplement to local anaesthetics the dose is only 10 – 20 µg.
These drugs are administered intravenously in continuous infusions. Due to tachyphylaxis and the rapidly changing status of the patient, the doses often have to be adjusted (titrated) often to achieve the goal.
Selective alpha 1 receptor agonists
Compounds
- Oxymetazoline
- Phenylephrine
- Xylometazoline
Indications
These drugs are used as nasal decongestants. Phenylephrine is also a vasopressor, used to treat hypotension.
Mechanism of action
These drugs are α1-selective agonists. They increase blood pressure by causing vasoconstriction. This vasoconstriction also decreases the swelling in the nasal mucous membrane.
Dosing
When used as nasal decongestants, these drugs are administered as a nasal spray.
Selective alpha 2 receptor agonists
Compounds
- Clonidine
- Dexmedetomidine
- Methyldopa
- Tizanidine
Indications
Methyldopa is used to treat hypertension in pregnancy, as it’s safe in pregnancy (unlike many other antihypertensive drugs).
Clonidine is used to treat spasticity, ADHD and hypertension, mostly in cases when the hypertension is acute.
Dexmedetomidine is used for sedation, during procedures or in case of agitated patients.
Tizanidine is used to treat spasticity.
Mechanism of action
All α2-selective agonists decrease blood pressure by acting on inhibitory α2-receptors in the vasomotor centre in the medulla oblongata. α2-agonism also gives them a muscle tone-decreasing effect, which is effective on spasticity, as well as a sedatory effect.
Methyldopa is a prodrug, meaning that it itself isn’t an alpha 2 agonist, but its metabolite methylnoradrenaline is.
Non-selective beta receptor agonists
Compounds
- Ephedrine
Indications
Ephedrine is used to treat nasal congestion, haemorrhoids, hypotension, nocturnal enuresis and to produce mydriasis.
Mechanism of action
Recall from the previous topic that ephedrine is an indirectly acting sympathomimetic, however it has some direct effects on β receptors as well.
Selective beta 2 receptor agonists
Compounds
These drugs are classified according to their duration of action.
- Short-acting beta 2 agonists (SABA)
- Salbutamol/albuterol (Ventoline®)
- Terbutaline
- Long-acting beta 2 agonists (LABA)
- Formoterol
- Salmeterol
- Ultra long-acting beta 2 agonist (ULABA)
- Vilanterol
Indications
The selective β2 agonists are mainly used as inhalations to treat asthma.
These drugs are also tocolytics, meaning that they relax the uterus. By relaxing the uterus they can be used to postpone labour.
Mechanism of action
Beta 2 agonists induce bronchodilation and dilation of the uterus.
Pharmacokinetics
All of these drugs have onset of action of 1 – 5 minutes, except salmeterol, which needs at least 30 minutes to work.
Selective beta 3 receptor agonists
Compounds
- Mirabegron
Indications
Mirabegron is used to treat overactive bladder.
Mechanism of action
Mirabegron is a selective beta 3 receptor agonist. This receptor mediates bladder relaxation (and stimulates lipolysis and thermogenesis).
According to the table ☝️ alpha1 receptor is present in the urinary bladder and sphincter; it makes since to use alpha1 agonists.
Thank you man for the amazing work! I wish the most successful exam period! Your fellow colleague❤️
I see the way that you’re thinking, but just because the theory matches up doesn’t meen practice does too. If you look up the treatment for nocturnal enuresis, alpha 1 agonists are not used.
Glad you like my work. Good luck to you too!
Hey!
Nocturnal enurisis should be treated with alpha 1 agonist, no
Nocturnal enuresis should actually be treated with desmopressin. Ephedrine is rarely used for that anymore. I don’t think alpha 1 agonists are used.
Oxymetazoline and xylometazoline, aren’t they non selective?
Not according to the book and amboss.