Table of Contents
Page created on March 5, 2018. Last updated on January 15, 2024 at 16:47
Learning objectives
- What is the substrate for the pentose phosphate pathway?
- What are the products of the pentose phosphate pathway, and what are they used for?
- Which other enzyme produces NADPH?
- Where does the PPP take place?
- What are the phases of the PPP?
- What is glutathione and what is its importance?
- What is the function of hexose 6-phosphate dehydrogenase?
- What are the 5 possible fates of glucose 6-phosphate?
- What is glucose 6-phosphate dehydrogenase deficiency, and why is it more prevalent in areas endemic to malaria?
- What is Wernicke-Korsakoff syndrome, and what causes it?
The pathway
The pentose phosphate pathway (PPP) is a metabolic pathway which takes place in the cytosol. It degrades glucose 6-phosphate and provides NADPH and pentoses.
NADPH is similar to NADH in structure (only a phosphate group differs), but they have very different biochemical roles. NADH serves as an electron carrier. It basically moving electrons from energy sources like glucose into the mitochondria, where the electrons NADH carry are used to generate ATP from ADP.
NADPH is used for anabolic reactions, meaning reactions where new large molecules, like fatty acids and steroids, are synthesised. NADPH is also used by the cytochrome P450 system in the liver, which we’ll learn about in biochem 2. It’s also a cofactor for glutathione reductase, the enzyme which recycles glutathione, an important antioxidant. Lastly, NADPH is needed for NADPH oxidase, an enzyme important for the oxidative burst. This is a process where neutrophils produce reactive oxygen species by NADPH oxidase, and uses these species to destroy phagocytosed pathogens.
Riboses are sugars which consist of five carbons. Riboses like ribose 5-phosphate are needed for synthesis of nucleotides, which are needed for the synthesis of DNA, RNA, FAD, NAD+, and coenzyme A. NADPH is also necessary to convert ribonucleotides (found in RNA) to deoxyribonucleotides (found in DNA), so it’s also necessary for DNA synthesis.
Some cells only need the NADPH and not the riboses. These cells can metabolise the riboses for energy, instead. Note that cells can also produce NADPH through an enzyme not part of this pathway, called malic enzyme.
The PPP occurs mostly in:
- The liver – which needs NADPH for fatty acid and cholesterol synthesis
- Adipose tissue – which needs NADPH for fatty acid synthesis
- Adrenal cortex, testis, ovaries – which need NADPH for steroid hormone synthesis
- RBCs – which need NADPH for glutathione reductase
- Neutrophils and macrophages – which need NADPH for NADPH oxidase
- Any rapidly producing cells – which need riboses and NADPH for DNA synthesis
- This includes the bone marrow, skin, mucous membranes, tumours
The PPP consists of two phases – one oxidative and one non-oxidative.
Oxidative phase
During the oxidative phase, molecules of G6P are oxidized to ribose 5-phosphate. This phase produces 2 NADPH. The enzymes in this phase that convert NADP+ to NADPH are glucose 6-phosphate dehydrogenase and 6-phopshogluconate dehydrogenase, which each yield 1 NADPH.
In some tissues, that need both NADPH and pentoses for nucleotide synthesis, the pathway stops here. However, there are tissues that only need NADPH and would rather use the pentoses for energy. That’s when the non-oxidative phase begins.
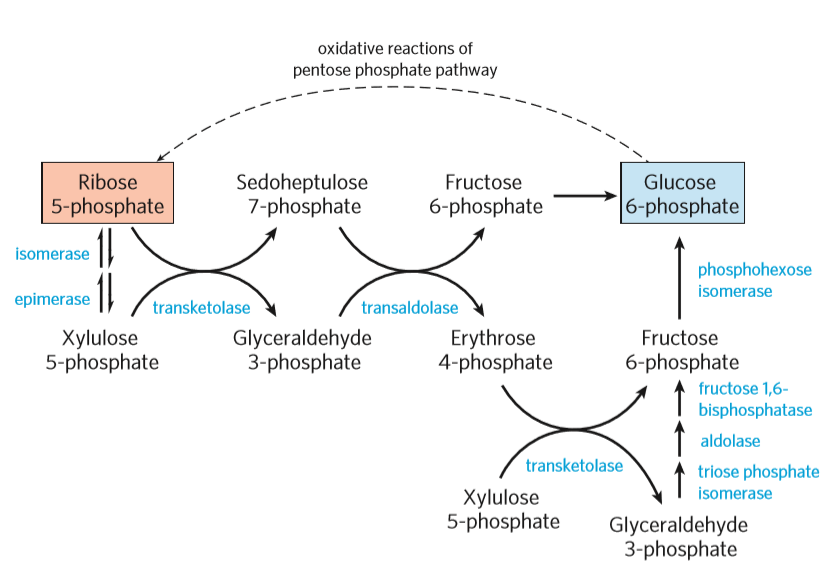
The non-oxidative phase of the pentose phosphate pathway. Note that transketolase can catalyse two similar, but different reactions. Check the MRTs.
Non-oxidative phase
During the non-oxidative phase, 6 molecules of ribose 5-phosphate go through a series of reactions to be converted to 5 molecules of glucose 6-phosphate, which can go through the oxidative phase again. The non-oxidative phases use multiple enzymes, two of which are exclusive to this pathway. Those are transketolase and transaldolase. The others are enzymes also used in gluconeogenetic or glycolytic pathways.
Transketolase and transaldolase both function by basically moving groups of H – C – OH between sugar molecules. See the MRTs for more details. Note that transketolase uses TPP as a cofactor and transaldolase doesn’t.
Some tissues don’t need NADPH and only needs pentoses. They can produce pentoses by running fructose 6-phosphate and glyceraldehyde 3-phosphate through the non-oxidative phase.
Regulation of the PPP
The pentose phosphate pathway is regulated by negative feedback. NADPH allosterically inhibits glucose 6-phosphate dehydrogenase. If the level of NADPH is high, glucose 6-phosphate dehydrogenase will be allosterically inhibited. If the level is low, the enzyme will be un-inhibited.
Fates of glucose 6-phosphate
Glucose 6-phosphate can have many possible fates, depending on the need of the cell and the body:
- It can be stored as glycogen
- This is called glycogen synthesis
- It can be oxidized to pyruvate
- This is called glycolysis
- It can be oxidized in the pentose phosphate pathway
- It can be used to build extracellular matrix
- It can be dephosphorylated into glucose and released into the bloodstream
- This is called gluconeogenesis
Hexose 6-phosphate dehydrogenase
The endoplasmic reticulum and sarcoplasmic reticulum have their own NADP+ and NADPH. These molecules can’t be transported across the endoplasmic or sarcoplasmic membrane, so these organelles must synthesize their own NADPH to maintain the reduction-oxidation balance. These organelles also need NADPH for steroid hormone synthesis.
The enzyme hexose 6-phosphate dehydrogenase produces NADPH in these organelles. It doesn’t use glucose 6-phosphate as a substrate but rather galactose 6-phosphate, glucose 6-sulphate, and glucose.
Glutathione
Glutathione is the most important antioxidant in the body. It’s synthesized from glutamate, cysteine and glycine. As an antioxidant glutathione can be oxidized instead of important components of the cell. Most importantly glutathione prevent oxidative damage to the RBC’s cell membrane, which would cause damage to the membrane.
Glutathione is written as GSH when in reduced form. This is the form where glutathione has antioxidant properties. When glutathione is oxidized, it’s oxidized to its oxidized form, GS-SG.
NADPH is required to reduce GS-SG back to the GSH form, which is why RBCs are dependent on a steady supply of NADPH to keep glutathione in the GSH form.
Glucose 6-phosphate dehydrogenase deficiency
Glucose 6-phosphate dehydrogenase deficiency (G6PD deficiency), sometimes called favism, is a genetic condition in which the body has reduced activity of glucose 6-phosphate dehydrogenase, and therefore can’t effectively produce NADPH. The biggest impact of this is that RBCs can’t produce enough glutathione and are therefore much more susceptible to oxidative stress.
RBCs of people with this condition are more vulnerable to oxidative stress than healthy people. In people with G6PD deficiency in periods of high oxidative stress, the membrane of the RBCs will lyse, causing haemolysis and resulting anaemai. The haemoglobin in RBC’s can be also degraded into so-called Heinz-bodies.
High oxidative stress can be triggered by certain drugs or viral or bacterial infection. Interestingly, a type of bean, called the Fava bean, also causes oxidative stress.
G6PD deficiency is most common in places where malaria is endemic, like in Africa and the Mediterranean. This is because G6PD deficiency has malaria resistance as a side effect, and there is therefore an evolutionary selective advantage for people with this disease in these areas. It’s X-linked recessive, so it mostly affects men.
The resistance occurs because cells that are infected by malaria are exposed to heavy oxidative stress, which kills the cells. This prevents the malarial parasite (plasmodium species) from multiplying and spreading.
Wernicke-Korsakoff syndrome
Wernicke-Korsakoff syndrome is a disorder caused by severe chronic thiamine (vitamin B1) deficiency. This occurs most commonly in chronic alcoholics, due to inadequate thiamine intake, dysfunctional absorption, and impaired storage of the vitamin in the liver of these persons.
The cofactor TPP is derived from thiamine. TPP is necessary for many enzymes in the metabolism of carbohydrates and amino acids. Thiamine deficiency causes ATP depletion as the body can’t break down carbohydrates or amino acids for energy. This affects the brain the earliest, which is the one of the organs with the most active glucose metabolism.
The syndrome can either present acutely or chronically. If it’s acute then the condition is called Wernicke encephalopathy, which is reversible. It causes sudden confusion, abnormal gait, among other problems.
Thiamine deficiency also causes chronic problems, called Korsakoff syndrome. This causes insidious memory loss and personality changed.
A defect in the gene for transketolase, which requires TPP to work, can give the enzyme a much lower affinity for TPP than normal. This is a very rare defect, but it makes patients much more sensitive to thiamine deficiency. Patients with this defect cannot tolerate even mild thiamine deficiencies, that healthy people could tolerate.
Summary:
- What is the substrate for the pentose phosphate pathway?
- Glucose 6-phosphate
- What are the products of the pentose phosphate pathway, and what are they used for?
- NADPH
- Used for steroid, cholesterol, fatty acid synthesis
- Used for glutathione recycling
- Used for oxidative burst
- Pentoses
- Nucleotides -> RNA, DNA, NAD, FAD
- NADPH
- Which other enzyme produces NADPH?
- Malic enzyme
- Where does the PPP take place?
- In the cytosol
- What are the phases of the PPP?
- Oxidative phase first, then the non-oxidative
- What is glutathione and what is its importance?
- It’s an antioxidant which mainly prevents oxidative damage to the RBCs membrane
- What is the function of hexose 6-phosphate dehydrogenase?
- It produces NADPH in the ER and SR
- What are the 5 possible fates of glucose 6-phosphate?
- It can be stored as glycogen
- This is called glycogen synthesis
- It can be oxidized to pyruvate
- This is called glycolysis
- It can be oxidized in the pentose phosphate pathway
- It can be used to build extracellular matrix
- It can be dephosphorylated into glucose and released into the bloodstream
- This is called gluconeogenesis
- It can be stored as glycogen
- What is glucose 6-phosphate dehydrogenase deficiency, and why is it more prevalent in areas endemic to malaria?
- It’s a genetic disease which decreases the NADPH synthesis
- It prevents against malaria, giving it an evolutionary advantage in malaria endemic areas
- What is Wernicke-Korsakoff syndrome, and what causes it?
- It’s a neuropsychiatric syndrome caused by ATP depletion due to thiamine deficiency
Hi,
In Regulation of PPP, shouldn’t it be ‘ If the level of NADPH is high, glucose 6-phosphate dehydrogenase will be allosterically INHIBITED’ not activated?
Biochemistry 1 is a long time ago, but I think you’re right. Good catch!
I have a question about the oxidative phase !
which reaction catalyze the actual oxidation?
It says in the text. The “glucose 6-phosphate dehydrogenase and 6-phopshogluconate dehydrogenase” enzymes.