Page created on October 7, 2018. Last updated on November 19, 2018 at 17:16
Bilirubin
Bilirubin is a breakdown product of the porphyrin rings of haemoglobin. Bilirubin is therefore a haemoglobinogenic pigment with a yellow-orange colour. It doesn’t contain iron.
Bilirubin is insoluble in water and is therefore transported by albumin to the liver, where the hepatocytes conjugate it with glucuronic acid by biotransformation. After it becomes conjugated it becomes more water-soluble, so the liver therefore pours it into the bile.
The bile is dumped into the gastrointestinal tract where bacteria convert the conjugated bilirubin to urobilinogen. Urobilinogen is then excreted by the feces.
If, for some reason, bilirubin levels in the blood should increase will the result be a pigmentation called jaundice.
Jaundice
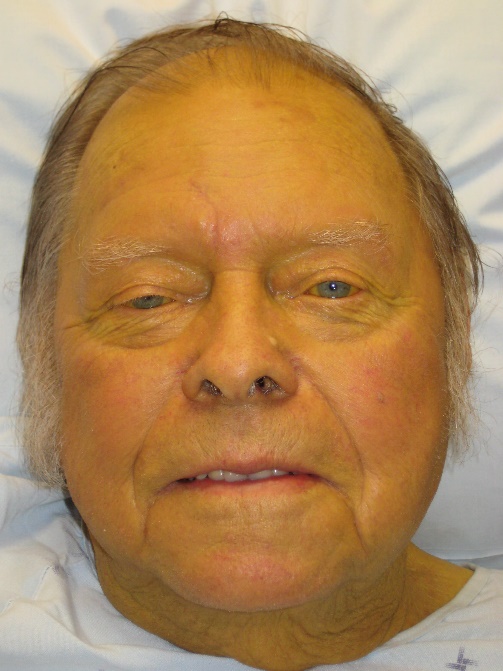
Jaundice, or icterus is a yellowing of the skin and sclera caused by hyperbilirubinaemia. The most common causes are
- Haemolytic anaemia
- The breakdown of haemoglobin increases
- Hepatitis
- Cholestasis
- Blockage of bile flow
- Neonatal icterus
- Jaundice in neonates is normal, as their bilirubin breakdown enzymes aren’t ready yet
- Gilbert syndrome
- A benign disease where bilirubin levels in blood are elevated but cause no harm
- Dubin-Johnson syndrome
- A defect in a liver transport protein causes harmless hepatomegaly and hyperbilirubinaemia
Jaundice itself isn’t usually harmful, however the condition that caused the jaundice often has other clinical consequences.
It is most commonly caused by cholestasis.
Cholestasis
The word comes from chole (= bile) and stasis (= staying still). It refers to any condition that affects bile formation or secretion, or a condition where the bile is obstructed. Cholestasis is usually caused by a dysfunction of the liver or an intrahepatic or extrahepatic obstruction of the bile ducts. Jaundice is usually the first symptom. Cholestasis can also present with skin xanthomas, which are yellow accumulations of cholesterol under the skin.
Jaundice is always an urgent sign that something is wrong, and the underlying cause must be treated. Extrahepatic biliary obstruction can be treated by surgery however intrahepatic obstruction cannot.