Page created on October 7, 2018. Last updated on April 27, 2019 at 15:31
Calcification is the pathological deposition of calcium in tissues. We distinguish two different types: dystrophic calcification and metastatic calcification.
Dystrophic calcification
Dystrophic calcification occurs in necrotic, injured or even dead tissues. It occurs with normal calcium level in the blood, meaning that hypercalcaemia is not a prerequisite for this type of calcification.
It begins with an initiation, which is when a calcium “core” is formed. Later will calcium continue to deposit on this core, a process called propagation. The result is the formation of crystalline calcium phosphate.
The initiation and propagation can take place either extra or intracellularly. Extracellularly the calcium core comes from degenerating cells and intracellularly it begins in the mitochondria of dying cells that are no longer able to regulate the intracellular calcium.
Dystrophic calcification is seen in these cases:
- Tuberculosis
- Caseous necrosis is a common area for dystrophic calcification
- Atherosclerosis
- The calcification that takes place in AS is dystrophic.
- Heart valve disease
- Aging or damaged valves will become calcified, which severely reduces its motion and causes stenosis.
- Adiponecrosis
- Cancer cells
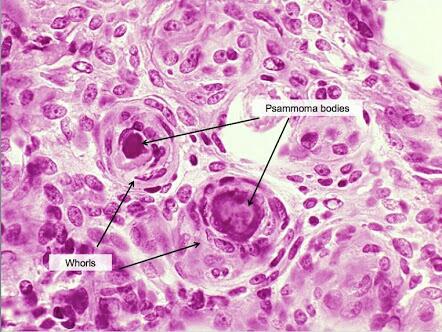
Psammoma bodies are concentric calcified structures commonly found in meningioma, thyroid carcinoma and ovarian carcinoma.
Metastatic calcification
In metastatic calcification calcium is deposited in healthy cells and tissues because of hypercalcaemia. Because of this it’s often seen throughout many tissues and is not localized.
Hypercalcaemia can be caused by:
- Vitamin D overdose
- Increased bone reabsorption
- Bone tumours
- Immobilization
- Osteoporosis
- Sarcoidosis
- Hyperparathyroidism
- Can be due to parathyroid tumour
- Kidney failure
- This results in phosphate retention, which leads to secondary hyperparathyroidism
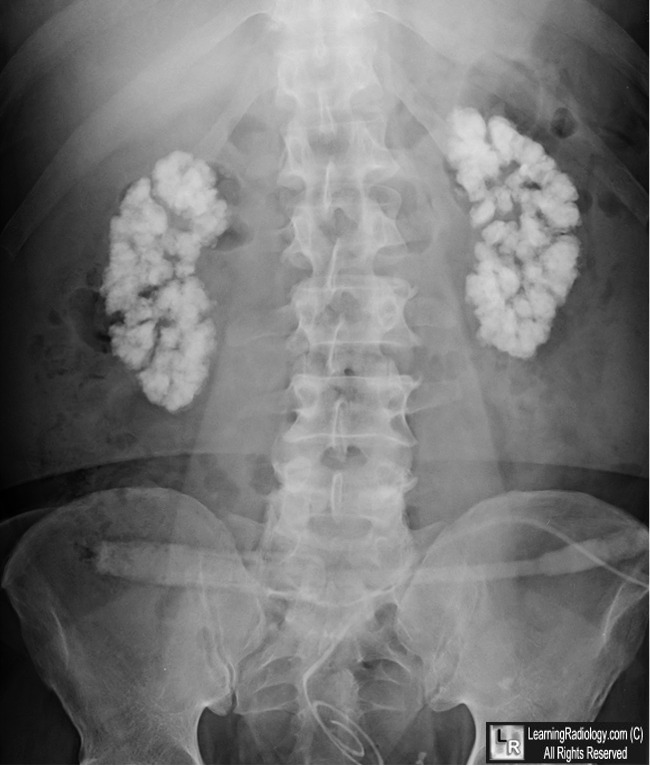
Metastatic calcification is usually seen in the vasculature, kidneys, lungs and gastric mucosa. It can cause respiratory problems and massive calcification of the kidney, leading to nephrocalcinosis.
Morphology
No matter the reason for the calcification will the morphology be the same.
On histological examination calcification appears as intra or extracellular basophilic deposits. In chronic calcification can even bone tissue be seen!
Macroscopically calcification looks like fine white granules or clumps.
Whore like structure?
Like you
«whorls” is a description of something circular. You can say that a Hassall corpuscle is a whorl shaped structure.
In persons with repeatedly asthma attacks, we can see mucous plugs in the bronchi. These plugs contains whorls of epithelium, also referred to as “Cursch Mann spirals”
Robbins path. 470
Thank you. I added a reference to your comment to the topic.