Table of Contents
Page created on October 22, 2018. Last updated on December 13, 2018 at 14:48
Thrombi
The definition of a thrombus (thrombi in plural) is intravascular coagulation of blood, meaning a solid mass of blood constituents.
A thrombus is firm, has fibrin on the surface and attaches to the wall. Lines of Zahn can also be seen, that are pale layers of fibrin and platelet and dark layers of red blood cells.
Recall from topic 1 that post-mortal clots are different from a thrombus.
Virchow’s triad
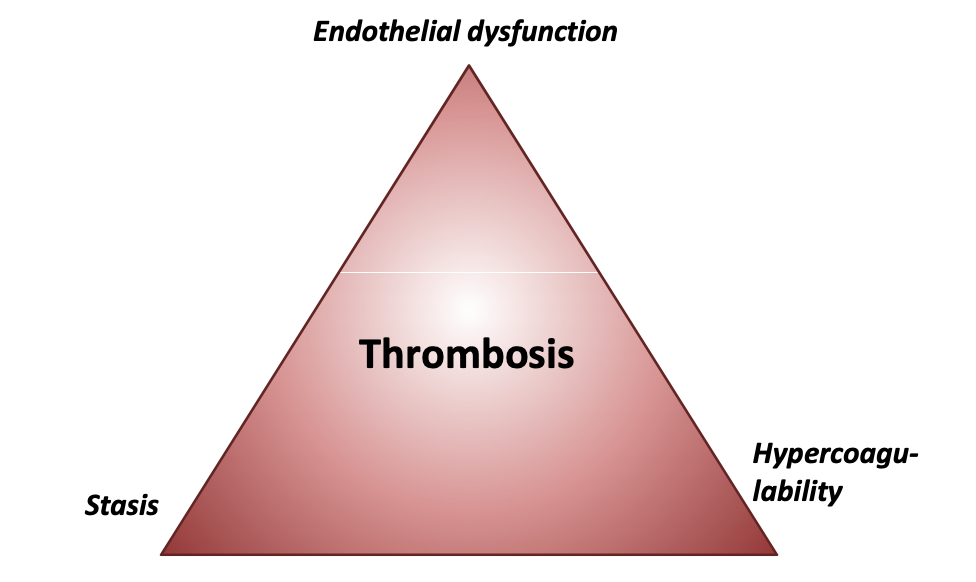
The Virchow’s triad represents the three broad categories that are thought to lead to thrombosis. We are going to take a more detailed look at all three.
Endothelial dysfunction
Healthy endothelial cells have both antithrombotic and prothrombotic properties. This balance is important but can be disrupted if there is any injury to the endothelium. Damaged endothelial cells produce greater amounts of procoagulants and stops synthetizing antithrombotic molecules, which tips the balance toward clotting. Risk factors for endothelial injury include:
- Atherosclerosis
- Vasculitis
- Smoking
- Hypertension
- Bacterial endotoxin
- Valvular disease
- Myocardial infarct
Stasis
Stasis means stopping of the blood flow. In normal laminar (= non-turbulent) blood flow, the platelets and other cell types are found in the center of the vessel lumen, separated from the endothelium by slower-flowing plasma. However, in turbulence and stasis, the platelets will come in contact with the vessel walls and can initiate clotting. It occurs in e.g.:
- Atrial fibrillation
- Venous obstruction
- Venous insufficiency
- Aneurysm
Hypercoagulability
Any alterations of the coagulation pathway that predispose to thrombosis. Here are some examples:
- Thrombophilia – abnormality where risk for thrombosis is increased.
- Estrogen-therapy – such as birth control pills or menopausal therapy.
- Antiphospholipid-syndrome
- Malignancy in cancer, like migrating thrombophlebitis (Trousseau’s sign)
- Deficiency of anticoagulant proteins as antithrombin III, protein C and protein S.
Classification of thrombi
A thrombus can either be red or white. The white thrombus is typical for arteries and consists mostly of platelets, while the red thrombus gets its color from the large red blood cell content since the blood flow in the veins is sluggish.
Location:
| Arterial thrombus | White thrombus due to atherosclerosis or vasculitis that rupture, and can be occlusive and block an artery, or mural and attach to wall. Grow in size towards the heart. |
| Venous thrombus | Red thrombus due to stasis. They are occlusive and grow towards the heart. |
| Cardiac Thrombus | This category includes thrombus of the auricle, atrial ball thrombus and of heart aneurysm and vegetation (bacterial growth on the heart valves, leading to a mass). |
| Microthrombi | Occur in capillaries and are red. |
Fate of thrombi
Five things can happen to the thrombus after its formation:
- Propagation – the thrombus enlarges by adding more platelets and fibrin, increasing the risk of occlusion or embolization.
- Embolization – Some part or the whole thrombus loosens from the vessel wall and moves in the circulation.
- Thrombolysis – If the thrombus is new, dissolution by fibrinolytic factors can completely dissolve it. However, this doesn’t work with older thrombi because of their extensive fibrin polymerization.
- Organization or recanalization – Endothelial cells, smooth muscle cells and fibroblasts can grow into older thrombi, and with time, even capillaries can recanalize in the thrombus. This can actually reestablish the continuity of the original lumen.
- Inflammation – as Phlebitis, which is an inflammation of veins.
Emboli and its types
What is the difference between a thrombus and an embolus? While a thrombus is attached to the wall, an embolus is an intravascular solid, liquid or gaseous mass that is carried by the blood to a site that is distant from its origin. However, the majority of emboli are dislodged thrombi.
We distinguish between many types of emboli:
- Thromboembolus – Dislodged thrombus
- Fat embolus – fat globules from bone marrow in long bones when they fracture.
- Amniotic fluid embolus – uncommon with 80 % mortality rate! Tears in the placental membrane allows fetal epithelial cells with high thromboplastin activity to enter maternal circulation.
- Air embolus – Gas bubbles that enter for example during surgery or decompression sickness (scuba diving)
- Atheroembolus – Atherosclerotic plaques rupture.
- Tumor-cell embolus – Tumor cells detach. Rare.
- Foreign body embolus – Fungal hyphae and talc are examples of this.
Now let’s take a closer look at thromboembolism since it’s the most common form for embolization.
Thromboembolus
Here, we again have different types
1. Systemic embolization
This often happens in arteries or the heart. For example, in aorta, thrombus in aneurysm or an atherosclerotic plaque can detach. In the heart, vegetation, atrial thrombus or ventricular mural thrombi can travel with blood.
In the brain, encephalomalacia can happen if the emboli find its way to the cerebral vessels. Kidneys, spleen and intestines are prone to infarction as well. Occlusion of blood flow to the lower extremities leads to gangrene
2. Pulmonary embolization
The source of a pulmonary embolism is often the veins, especially from the lower extremities and pelvis, also called a deep vein thrombosis, DVT. Another source can be the right side of the heart, but this happens rarely.
A total pulmonary embolus completely occludes the pulmonary trunk, while a subtotal pulmonary embolus occludes only left or right pulmonary artery. However, both lead to right sided heart failure and possibly quick death.
Partial pulmonary embolus occludes a segmental artery and can in rare occasions lead to pulmonary infarct.
3. Paradoxical embolization
In atrial or ventricular septal defects can a mixture between the two types discussed earlier can happen. A DVT can turn into a systemic embolization and an arterial thrombus can suddenly end up as a pulmonary embolism.
Thanks for the great work! Cool blog. There are several opinions on this topic and this blog states the problem extremely great.
I wasn’t aware that there are several opinions on the topic of definitions, causes, types, and clinical consequences of thrombosis and embolus.