Page created on September 16, 2018. Last updated on November 19, 2018 at 17:16
In liquefactive necrosis the tissue is turned into a liquid mass, hence the name. Common for all types of liquefactive necrosis is that the cells are completely digested by enzymes, which results in a soft lesion consisting of fluid remains of necrotic tissue. We have two main types, encephalomalacia and abscess formation.
Encephalomalacia
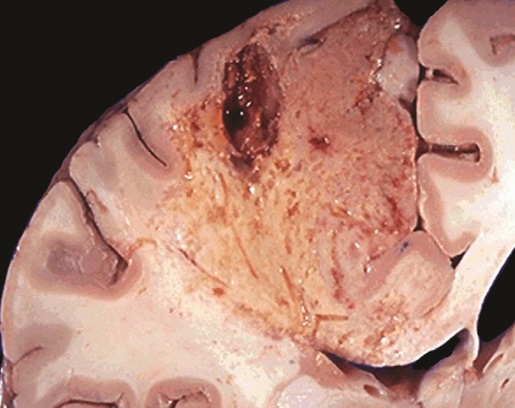
Also called cerebral infarct, encephalomalacia (from encephalo = brain, and malacia = softening) occurs when parts of the brain are ischemic. For reasons unknown, tissues in the CNS that die because of hypoxia always results in liquefactive necrosis. Over time, a cyst will be formed.
We distinguish three types of encephalomalacia. The pale or white type occurs in white matter due to a thrombus. The red or haemorrhagic type occurs in grey matter due to an embolus. The yellow type is actually a weeks old infarct.
Abscess
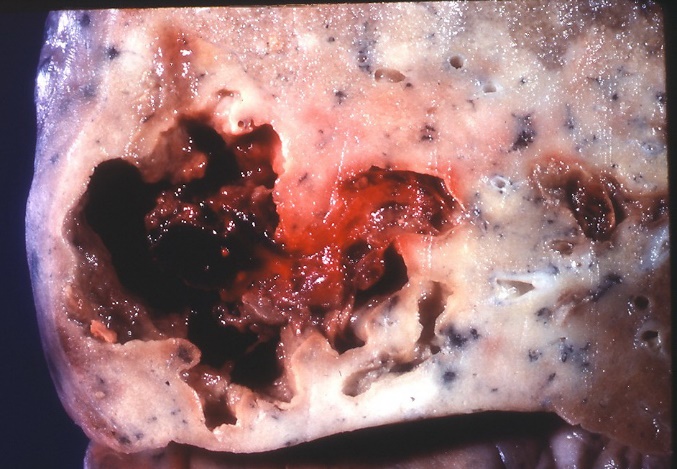
Pathogens that can cause abscess formation are called pyogenic pathogens. In abscess formation, the fluid remains are not only comprised of necrotic tissue debris, but also pus. Pus consists of neutrophils, necrotic cell debris and edema fluid. The abscess can either be caused by the pyogenic infection itself, or by a secondary infection of already necrotic tissue.
In an abscess there is always a pyogenic membrane which surrounds the purulent inflammation. The membrane prevents the infection from spreading to other tissues.
Like wet gangrene, abscesses must always be removed because the pyogenic membrane can fail, which can lead to sepsis.
Abscess formation is common in the lungs, brain and the liver.
Is it common for the spleen to liquify postmortem?
Good question, I do not know
May I ask what is difference between Abscess formation and Wet Gangrene?!
I’d be GLAD to explain it to you, John Cena.
An abscess is a circumscribed lesion, demarcated from the surrounding tissue by the pyogenic membrane. It usually contains liquid-like pus and necrotic tissue.
Wet gangrene is the result of saprophytic organisms infecting and feeding on already dead tissues. It’s not sharply demarcated from surrounding tissue.