Table of Contents
Page created on February 23, 2019. Last updated on May 4, 2022 at 11:54
Written by ms. worldwide, edited by Nikolas.
The appendix
The vermiform appendix is a true diverticulum of the cecum, and like any diverticulum, its prone for acute and chronic inflammations. The most common pathology in the appendix is acute appendicitis, but tumors can also occur there.
Acute appendicitis
Introduction and epidemiology
Acute appendicitis refers to acute inflammation of the vermiform appendix and is a common cause of acute abdomen. Rapid management is important to prevent complications such as perforation of the appendix.
The lifetime incidence of appendicitis is 9% for men and 7% for women. The peak incidence is in the second and third decades of life, but it may occur at any age. The incidence of acute appendicitis has been decreasing since the 1970s, for reasons not known.
Etiology and pathomechanism
The etiology of acute appendicitis is largely unknown; it frequently occurs in healthy, young people. Outside age, gender, and family history, no real risk factors are known.
In most cases, an obstruction is identified, but not always. Obstruction may be caused by hard faecal masses, calculi, lymphoid tissue hyperplasia, or tumours. An obstruction may lead to increase in luminal and intramural pressure, which may cause thrombosis in small vessels, causing localised oedema. The obstruction of the venous outflow leads to ischemic injury and stasis of luminal contents. This gives bacteria a perfect place to proliferate in, which in turn will trigger the inflammatory responses. Tissue edema and neutrophilic infiltration of the lumen, muscular wall and periappendiceal tissue will take place. The pathological criterium to diagnose acute appendicitis is neutrophilic infiltration of the muscularis propria. In more severe cases, focal abscesses may form within the wall, and this is then called an acute suppurative appendicitis. These may also progress to large areas of hemorrhagic ulceration and gangrenous necrosis, into an acute gangrenous appendicitis, which is often followed by rupture and resulting peritonitis.
Clinical features
Localised appendiceal oedema stimulates visceral afferent pain fibres, initially leading to vaguely localised periumbilical abdominal pain. Later, the inflammation will involve the adjacent parietal peritoneum, causing the characteristic peritonitic pain in the right lower quadrant.
The classical symptoms are:
- Initial diffuse periumbilical pain which evolves into peritonitic pain at McBurney’s point
- Anorexia (decreased appetite)
- Nausea and vomiting
Treatment
Treatment is surgical removal of the appendix, appendectomy, usually performed laparoscopically.
Chronic appendicitis
Chronic appendicitis shows the same symptoms as the acute one, but much milder. The symptoms also come and go, and this can last for weeks, months or years. Many times, it’s also not diagnosed until it becomes an acute appendicitis.
Tumors of the appendix
Tumors in the appendix are rare, but we will discuss them anyway.
The most common found in the appendix is the carcinoid, also known as a neuroendocrine tumor, and its usually discovered during resection surgery of an appendix. This type of neoplasm is usually seen on the distal tip of the appendix, like a yellow, solid swelling. Metastasis to lymph nodes and more distantly is very rare, even when intramural and transmural invasion is often seen. Since it’s a neuroendocrine cancer, it produces the hormones histamine, kallikrein, prostaglandins and serotonin when well differentiated.
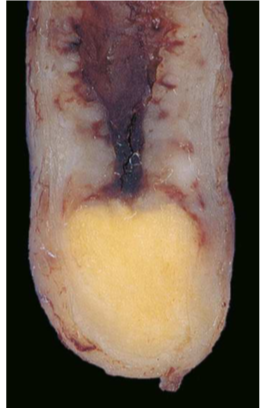
Carcinoid of the appendix. Notice how yellow and solid it is, and that it is located in the distal tip.
Conventional adenocarcinomas and non-mucin-producing adenocarcinomas can also occur in the appendix and mimic the way acute appendicitis presents which obstruction and enlargement of the appendix.
Mucocele is a dilated appendix filled with mucus and can be caused by an obstruction and contain thickened mucus. Or it may be a consequence of mucinous cystadenocarcinoma. The latter one can invade through the wall of the appendix and lead to intraperitoneal seeding. In the most severe cases, this spread can lead to pseudomyxoma peritonei which you can read more about below.
Peritoneal diseases
Peritonitis
Peritonitis is the inflammation of the peritoneum. It may be localised or generalised. Peritonitis is a clinical diagnosis, established by the presence of typical clinical findings, like rebound tenderness, guarding, and pain on gente percussion. Rebound tenderness refers to the phenomenon where the patient feels pain when you quickly remove pressure from the abdomen, while guarding refers to involuntary contraction of abdominal wall muscles when palpating. The patient is usually in severe pain and lies completely still because movement worsens the pain.
The cause for peritonitis is usually infectious, caused by bacteria. It may be primary (rare) or secondary (more common). Primary peritonitis occurs due to bacterial infection of ascitic fluid (called spontaneous bacterial peritonitis), while secondary peritonitis is more frequent and occurs due to perforation or inflammation of adjacent abdominal organs, like appendicitis, pancreatitis, cirrhosis, etc.
Peritonitis is a severe condition because it can lead to paralytic ileus or adhesions of organs, or sepsis. Secondary peritonitis is a sign of underlying severe disease which may be life-threatening.
Retroperitoneal fibrosis
Ormond’s disease, also known as retroperitoneal fibrosis is a condition characterized by the development of extensive fibrosis throughout the retroperitoneum. The exact pathogenesis is unknown but may be related to an immune response against atherosclerotic plaques. Fibrosis usually begins around a severely atherosclerotic aorta. It’s also associated to certain autoimmune disorders like Sjögren and Crohn disease. It can also occur as a result of trauma, radiation or certain drugs.
The condition presents with nonspecific symptoms like dull pain in the back. The fibrosis may envelop retroperitoneal structures like the inferior vena cava or ureter, potentially causing renal failure.
Pseudomyxoma peritonei
This condition, often called PMP, is a rare (1-2 cases per million people) condition of the peritoneum. It begins with an adenocarcinoma or mucinous cystadenocarcinoma in the appendix which perforates the wall of the appendix and spreads to the peritoneum. The tumor cells multiply and continue to produce mucin which fills the peritoneal cavity. The increased abdominal pressure can obstruct the intestines.
Read it a bit fast, saw now that mucocele is covered. My mistake!
Hey!
Just wanted to say that this topic has a bracket behind it, where some of the content is not covered here. The bracket says appendicitis, mucocele, peritonitis, retroperitoneal sclerosis, pseudomyxoma of the peritoneum.
If retroperitoneal sclerosis is the same as retroperitoneal fibrosis, then it is only mucocele that is not covered.
Thanks for your good work, just wanted to say in case some people were not aware of it:)