Table of Contents
Page created on February 20, 2019. Last updated on May 4, 2022 at 14:15
Written by ms. worldwide, edited by Nikolas.
Congenital malformations
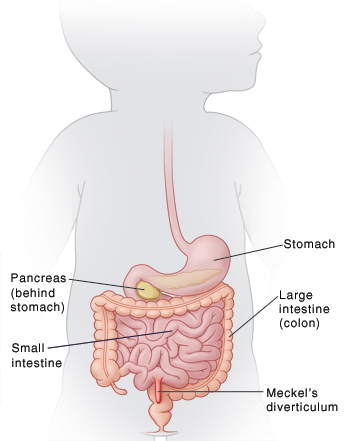
Meckel’s diverticulum
Meckel’s diverticulum is a remnant of the omphaloenteric/vitellointestinal duct and can be found in 2 % of the population. It is considered a true diverticulum, as it includes all the three layers of the intestinal wall.
Where is it found and how big can it be? It’s usually found as an outpouching from the ileum, on the antimesenteric side, approximately a half meter proximal to the ileocecal valve. It can range from 1-12 cm in length!
In ca. 10 % of the cases, even ectopic gastric or pancreatic tissues can be found in the diverticulum.
The diverticulum is mostly symptomless, but ulceration, bleedings and perforation can happen. Ulcerations happens usually due to ectopic gastric tissue, where acid is produced which harms the ileum.
Atresia and stenosis
This includes everything which leads to obstruction, like stenosis of the small intestine, abnormal rotation or even missing portions.
Malrotation
Normally, the physiological herniation of the intestines happens, where the intestines rotate 270 degrees counter clockwise. If this fails, we have a malrotation of the small intestines.
Circulatory disorders
Recall that the small intestine is supplied by the mesenteric arteries.
Mesenteric infarction
This happens if there is any occlusion of the mesenteric artery or one of its branches. Recall from pathology 1 that this is a very deadly situation. The infarction can be divided into mucosal, mural (mucosa + submucosa) or transmural infarction, based on how extensive the ischemia is. The transmural one is often caused by acute obstruction of an artery.
Causes for infarction in the bowels can be:
- Severe atherosclerosis
- Aortic aneurysm
- Hypercoagulative states
- Oral contraception
- Emboli from cardiac vegetations
- Systemic vasculitis
- Cirrhosis or portal hypertension that compress the portal drainage.
Non-occlusive intestinal ischemia
Decreased blood flow to the intestines can also happen in situations where there is no occlusion, like in:
- Shock
- Cardiac failure
- Use of vasoconstrictors
Short bowel syndrome
Short bowel syndrome is a malabsorption disorder caused by the lack of enough functional intestine. The causes for this are surgeries, where big portions of the small intestine get resected, like in Crohn’s disease or traumas.
Following the resection, the bowels undergo morphological and functional changes to compensate for the lost function, like enlargement and lengthening of villi and slower peristalsis. These changes are mediated by hormones, cytokines and growth factors.
The patients must take supplementary vitamins and eat small meals low on fat to get sufficient absorption of nutrients.
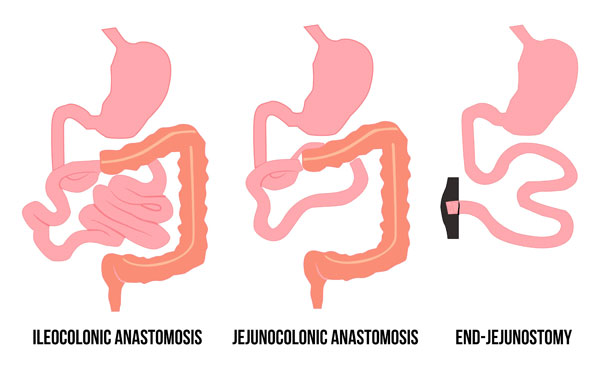
Reasons for short bowel
Inflammatory disorders of the small intestine
Infectious enteritis
Enterocolitis can manifest with a broad range of signs and symptoms including diarrhea, abdominal pain, urgency, perianal discomfort, incontinence, and hemorrhage.
Viral enteritis are probably the most common ones and is caused by the Rota- and Noroviruses.
The bacterial enteritides include:
- Cholera
- Salmonella
- Intestinal tuberculosis
- Whipple’s disease
- Pathogenic E. coli enteritis
Parasitic and protozoon enteritis is not as common as the viral and bacterial ones, but still infect people all the time, with e.g. tapeworms. The most common pathogenic parasitic infection is by Giardia lambia, causing giardiasis. It spreads by fecally contaminated water and food and is resistant to chlorine. Eww, a new reason to get paranoid when swallowing pool water by accident.
Whipple’s disease is an extremely rare chronic multisystem disease, affecting the small intestine. It is caused by the bacterium Tropheryma Whipplei. The most characteristic symptoms of it is called the classic triad and include:
- Abdominal pain and diarrhea
- Weight loss
- Arthritis
This disease can also affect the heart, lungs, brain and the eyes. However, its curable with long term antibiotic treatment. In histology, sickle particle containing cells can be seen.
Celiac disease
Celiac disease is also known as the celiac sprue or gluten-sensitive enteropathy and is an immune-mediated enteropathy. The trigger is ingestion of gluten-containing foods, like wheat, rye and barley. Gluten itself is a complex protein, containing e.g. glutenin and gliadin.
The causes for celiac disease are the genes HLA-DQ2 and HLA-DQ8. However, celiac disease can occur in persons without those alleles as well. Other immune diseases can also cause it, like diabetes mellitus type 1, Sjögren disease and thyroiditis.
When gluten is digested, it will be degraded in the intestines. The gliadin-molecule is however unable to be digested by our bodies and will only become deaminated. The deaminated gliadin then interacts with the HLA-molecules on antigen-presenting cells. In individuals with the HLA-DQ2/HLA-DQ8 allele, gliadin will be recognized as a pathogen by the CD4+ and initiate an immune response. Cytokines by CD4+ cells will cause damage of the mucosa, and CD8+ cells not specific for gliadin accumulate as well and cause damage. B-cells response follows and results in formation of anti-deaminated gliadin antibodies.
Celiac disease manifests in children with diarrhea, weight loss, abdominal pain, anorexia, muscle wasting, bloating and nausea. Some may even have blistering skin lesions, dermatitis herpetiformis.
In adults, it can be symptomless or cause anaemia, diarrhea, bloating and fatigue.
Patients with celiac disease are prone to enteropathy-associated T-cell lymphoma, which is an aggressive cancer.
This disease is however easily treated with a gluten-free diet.
To classify the grade of Celiac disease, the Marsh system is used. More can be studied in the slide section.
Lactose intolerance
The lactose intolerance manifests as a decreased or as a complete absence of the lactase production. The enzyme lactase is needed to cleave lactose into glucose and galactose.
Two forms of it has to be known here: the congenital and the acquired lactose intolerance. The congenital is due to a recessive autosomal disorder which mutates the gene for lactase. This disease is rare and can be lethal for new-borns because they only feed on mothers’ milk, which contains a lot of lactose and suffer from diarrhea. A substitution for mother’s milk should be given.
The acquired type is much more common and can be found in whole populations. In Asia, almost everyone suffers from lactose intolerance. This type is caused by the downregulation of the lactase gene after childhood, when mother’s milk is no longer needed.
It is a boring intolerance to have because you have to stay away from that McDonalds milkshake and McFlurry. 🤙
Tumors of the small intestine
All the tumors in the small intestine are very rare. Basically every GI-tract neoplasm can occur in the small intestine, like adenoma, adenocarcinoma, NET, GIST and intestinal lymphomas. The adenocarcinomas in the small intestine are often associated with Crohn’s disease.
Lymphomatous polyposis is also very rare and is found in the ileocecum. It has a poor prognosis.
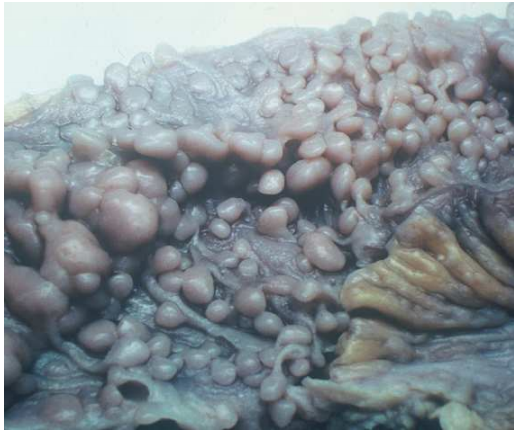
Lymphomatous polyposis
Hey,
The circulatory and inflammatory disorders, do they lead to malabsorption?
The circulatory disorders are acute and potentially life-threatening, so whether they cause malabsorption or not isn’t really relevant. The inflammatory ones do. Tbh I don’t know why the circulatory disorders are mentioned in this topic.