Table of Contents
Page created on May 3, 2019. Last updated on October 14, 2021 at 17:04
Introduction
The terminal duct lobular unit (TDLU) is the functional unit of the breast. Like the name suggests it’s comprised of a lobule + the terminal duct that lobule empties into. The lobule produces milk, and the duct carries that milk to the nipple. 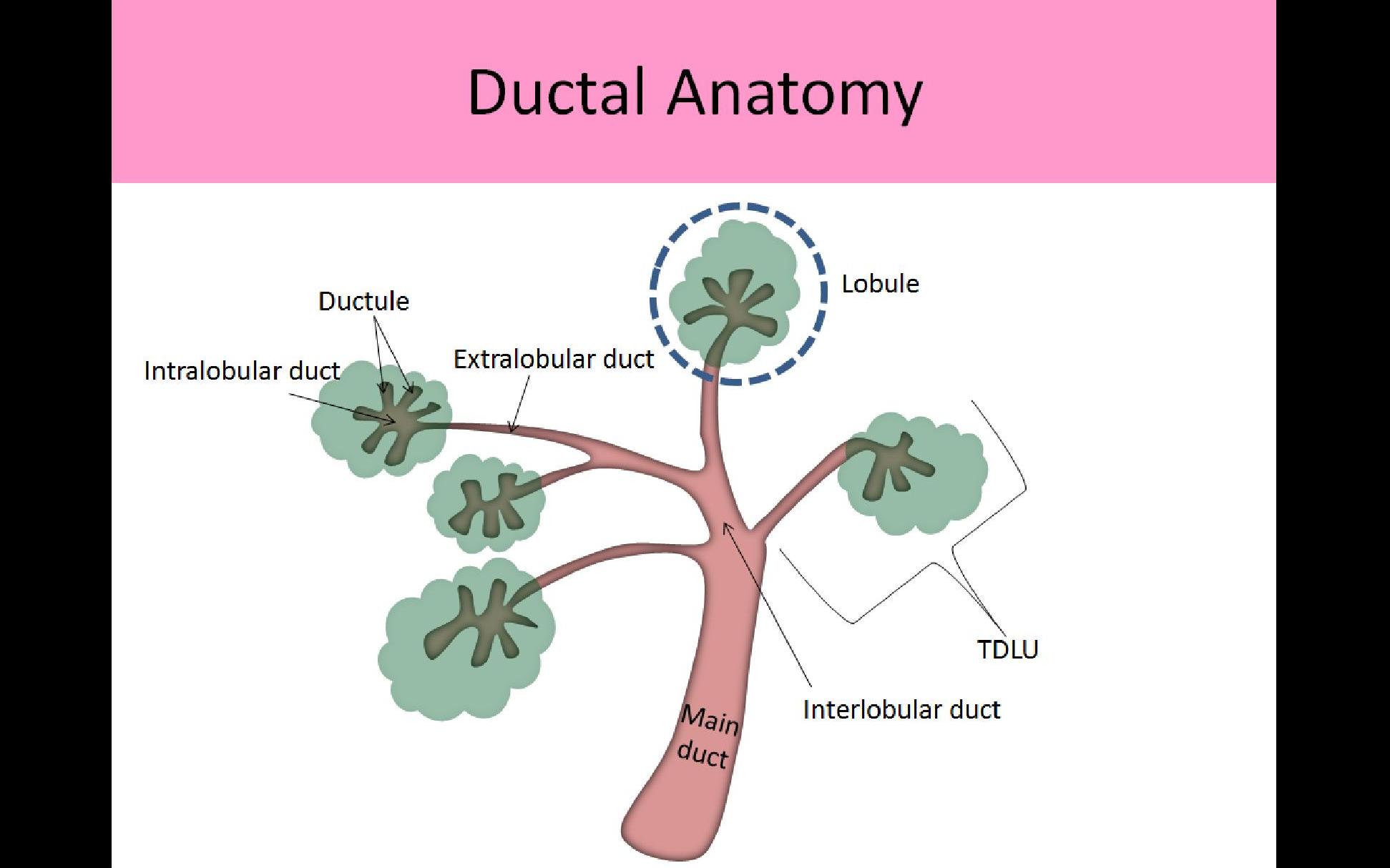
From https://ultrasoundregistryreview.com/BreastTrial4.html
All ducts and lobules of the breasts have two cell layers. The first layer is the luminal cell layer that faces the lumen, and the second layer is a myoepithelial layer.
The TDLU is important because it is from here breast tumors originate from.
Mastitides
Inflammation of the breast is called mastitis. It’s associated with redness, oedema, pain and tenderness of the breast, as well as fever. It may be infectious or non-infectious.
There are several subtypes of mastitis:
Lactational mastitis
Lactational mastitis occurs in lactating mothers who, for various reasons, can’t lactate enough, causing milk stagnation in the breast. This allows organisms to grow in the stagnant milk, causing infection. The most common organism is staphylococcus aureus. Bacteria enter the breast through fissures in the skin that develop during breastfeeding.
Treatment involves symptomatic treatment (painkillers, cold compresses) and emptying of the breast. Antibiotics may also be used.
Mammary duct ectasia
Mammary duct ectasia (plasma cell mastitis) is a non-bacterial lymphoplasmacytic inflammation of the breast that occurs in older, non-breastfeeding women. The etiology and pathogenesis is unknown, but as the name implies the ducts are dilated.
Extravasation of breast secretions from the ducts into the periductal connective tissue occurs, which forms a periareolar mass that can mimic cancer. The condition is harmless, although it produces a green nipple discharge.
Fat necrosis
Fat necrosis of the breast is a non-bacterial, non-neoplastic condition that occurs after trauma to the breast. A firm mass is formed, which may mimic cancer. This necrotic debris may also calcify, which can be visualized on mammography.
Galactocoele
Galactocele is a breast milk-containing cyst that occurs in young, lactating women. It occurs due to an obstructed milk duct. Like most conditions in this list it must be distinguished from cancer.
Mastitis carcinomatosa
Mastitis carcinomatosa (inflammatory breast carcinoma) is a type of breast cancer that manifests with an inflamed breast. It should be considered in patients with mastitis which doesn’t resolve with antibiotic therapy.
Fibrocystic changes
Introduction
Fibrocystic changes in the breast refers to multiple conditions where the terminal duct lobular unit is cystically dilated and fibrotic. These changes happen in women in the reproductive age and can even be thought of as part of physiological aging as they rarely cause problems. These changes are benign in themselves, but some may have an increased risk for progressing into carcinoma. If the change shows atypia the risk is even higher.
These changes are clinically relevant as they must be distinguished from breast cancer. In fibrocystic changes myoepithelial cells are present, unlike in breast cancer.
Fibrocystic changes are divided into non-proliferative and proliferative patterns. Of the latter group epithelial hyperplasia, sclerosing adenosis and complex sclerosing lesion are important.
Non-proliferative fibrocystic changes
Non-proliferative fibrocystic changes are the most common of the two types. There is formation of cysts and an increase in fibrous stroma. There is no epithelial hyperplasia. The cysts range from < 1 cm to 5 cm in diameter. They are typically blue, hence the nickname “blue dome cysts”.
Proliferative fibrocystic changes
Epithelial hyperplasia is a proliferative fibrocystic change characterised by hyperplasia of the two epithelial layers of the terminal duct lobular units. If there is atypia the condition is called atypical ductal hyperplasia (ADH) or atypical lobular hyperplasia (ALH), depending on whether the ducts or lobules are affected. These conditions are precursors for DCIS and LCIS, described in the next topic.
Sclerosing adenosis is a proliferative fibrocystic change characterised by an increase in glands and stroma. The glands are compressed by the surrounding stroma. These changes may cause calcifications, which can be visualized on mammography.
Complex sclerosing lesion is a proliferative fibrocystic change characterised by a stellate architecture with prominent fibroelastosis and epithelial hyperplasia. It forms nodules that can cause skin retraction and palpable nodules. These should be removed due to an increased risk of malignancy.
Fibroepithelial tumors
Fibroadenoma
Fibroadenoma is the most common benign neoplasm of the breast. They’re comprised of neoplastic fibroblastic stroma and normal glands. They’re most frequent in women 20 – 30 years of age. They form firm solitary, mobile, off-whitish well-circumscribed masses. As they are benign they aren’t necessary to remove.
Phyllodes tumour
Phyllodes tumour are similar to fibroadenomas, however their stromal component is more cellular. The name “phyllodes” comes from the Greek word for “leaf-like”, as the stroma often forms leaflike projections. They’re much less common than fibroadenomas. 75% of these are benign, and the remainder are malignant. As they have malignant potential they should be surgically removed.
Intraductal papilloma
Intraductal papilloma is, like the name suggests, a papillary growth that occurs inside dilated ducts. They’re more frequent in premenopausal women. The lesions are small (< 1 cm) and usually solitary. These tumors cause bloody nipple discharge.
These should be removed due to an increased risk of malignancy.