Table of Contents
Page created on September 29, 2018. Last updated on November 15, 2021 at 21:45
I recommend reading through topic 6 of internal medicine for a better introduction to this topic.
General
Syncope (or fainting) is a sudden, completely reversible loss of consciousness due to an acute reduction of cerebral perfusion. It may last from several seconds up to minutes. It occurs exclusively in orthostatic (standing or sitting where the head is up) posture. Along with the loss of consciousness is there also a loss in skeletal muscle tone, which causes the affected person to fall and assume a supine position where the circulation normalizes and consciousness is regained.
It’s important to note that not all cases of loss of consciousness are cases of syncope. A coma for example isn’t a type of syncope even though both include loss of consciousness.
Circulatory adaptation
In standing position, when blood pressure at the level of the heart is 120/80 mmHg, is the MAP:
- At the level of the heart: 80-100 mmHg
- At the level of the head: 60-80 mmHg
- At the level of the feet: 180-190 mmHg
This high MAP in the lower extremities means that there is a tendency for blood to pool there. Vascular adaptation in the legs is the key to maintaining cerebral blood flow, and therefore, when standing up after supine posture, the body must adapt and increase the vascular tone in the legs. When standing up, the baroreceptor-triggered sympathetic reflex mechanisms will react, and cause either arteriolar or venous constriction. This is called immediate adaption and prevents a sudden drop in venous return to the heart and blood pressure, and ensures that enough blood will flow to the brain.
Orthostatic syncope
If syncope occurs right after standing up from supine position, the condition is called orthostatic syncope. This is often due to an impairment of the immediate adaptation, which is often seen in elderly. Elderly have decreased sensitivity of the baroreceptors, which impairs the immediate adaptation.
Vasovagal syncope
Vasovagal syncope is the most common cause of syncope. Like the name implies the circulation and vagus nerve are involved. It occurs when the body overreacts to certain triggers, such as the sight of blood or extreme distress.
Etiology:
- Strong psychogenic effects
- Strong emotions
- Severe pain
- Fear
- Smell of blood
- Sight of blood
- Heat exposure
Something causes the vagus nerve to be overactivated. The vagus nerve causes bradycardia and systemic vasodilation. Vasodilation causes the blood pressure and venous return to decrease suddenly. This causes a massive but temporary hypoperfusion of brain, which results in a syncope with loss of consciousness.
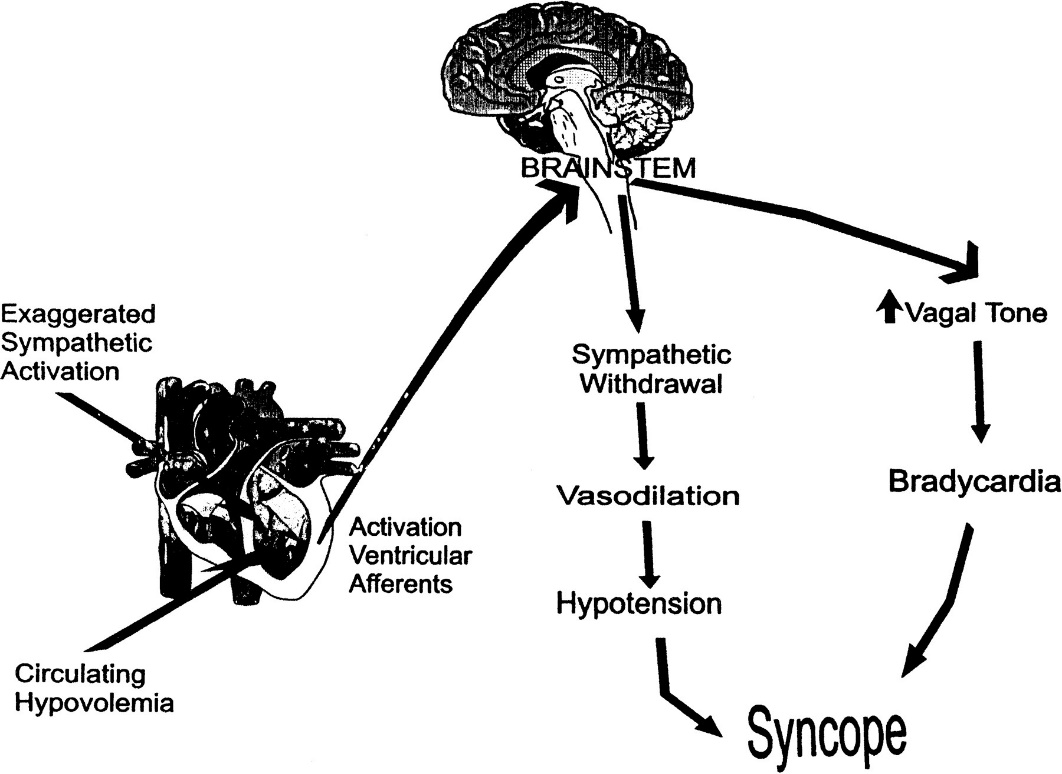
After loss of consciousness you will lose muscle tone, causing you to fall and assume a supine position. This evens out the distribution of blood, causing consciousness to be quickly regained. There will be no later symptoms. However, if you for example faint while sitting in your bed and don’t fall to a supine position the cerebral hypoperfusion will remain and severe symptoms can develop.
The cortex is the least-perfused part of the brain, so it’s affected the most by this. In fact, a 5-minute-long cerebral hypoperfusion causes the cortex to die completely, causing decortication syndrome!
Try to google “decortication syndrome” literally and note how the term hasn’t been used since the 60s.
Precollapse
Before vasovagal syncope occurs people often experience precollapse, a collection of symptoms related to decreased cerebral perfusion. Common symptoms include:
- Blackening vision
- Sounds becoming faint
- Nausea
- Pallor
- Diaphoresis (sweating)
- Lightheadedness
If you ever felt like fainting but lie down just before it happens, you may have experienced that you regain consciousness and feel better shortly after lying down. That is because the supine position improves the venous return and the cardiovascular parameters, and the brain finally gets enough blood.
Factors increasing the risk for syncope
Syncope is more expected in:
- people whose immediate adaptation is impaired
- people that have diseases giving them hypotension
- pregnancy, where there is a physiological decrease in blood pressure (usually around 110/70)
Other factors may be:
- Exhausting exercise (vasodilation)
- Valsalva maneuver
- Loss of blood
- Obstruction in venous return
- Sympathectomy
- Some drugs and medicines
- Hyperventilation