Page created on October 5, 2018. Last updated on October 18, 2020 at 10:11
Physiological splanchnic circulation
The GI-tract, liver, pancreas and spleen all together receive about 1.3-1.4 L/min which is 27% of the blood flow. Of this value, 300-350 mL goes to the hepatic artery alone.
The gastrointestinal motility and the secretion and absorption are all highly dependent on the organs involved receiving enough blood.
In response to food intake will the blood supply of these organs be increased. This increase is mediated by the hormones cholecystokinin (CCK), secretin and vasoactive intestinal peptide (VIP), along with kinins like bradykinin and kallidin.
Disorders of splanchnic circulation
When there is an impairment of the gastrointestinal circulation, the cells on the tip of the villi will be the first to be affected. This is because of the countercurrent blood flow inside the villi. The apical part of the villi is mainly responsible for absorption, so in the cause of circulation impairment, the absorption is the first function to deteriorate.
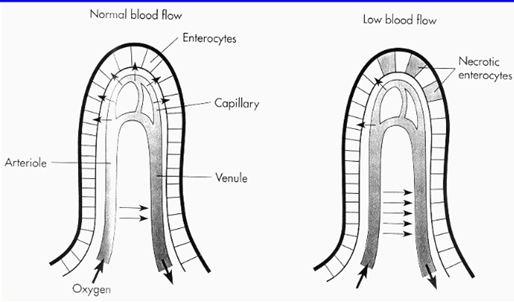
While absorption is impaired first, secretion and motility will be maintained as normal for a while. Later the motility will be impaired as well, potentially causing subileus.
In the case of ischemia of the pancreas will pancreatic proteolytic enzymes be released. A peptide called myocardial depressing factor (MDF) will also be released by the pancreas, which causes decreases the myocardial contractility.
Most of the arterial blood flow through the abdominal organs drain into the portal vein, which empties into the liver. This adds up to approximately 30% of the cardiac output flowing through the liver. Therefore, many disorders of the liver easily can impair the filling of the heart, and a failing heart often gives symptoms in the liver.
It’s important to keep in mind that if there is any need for redistribution of the circulation will blood always be directed from the splanchnic areas to the areas that need more blood, like the brain, muscles or skin.
Hi N,
Can we consider the blood running through the portal veins a part of the CO? I’m just wondering if it’s correct to say that 30% of CO run through hepatic veins. 🙂
Who is N?
I’ve rewritten the paragraph to be more precise.
Awesome 🙂
You’re N (sorry I was in a hurry) 🙂